 Qaseem A, Kansagara D, Forciea MA, Cooke M, Denberg TD, Clinical Guidelines Committee of the American College of P (2016) Management of chronic insomnia disorder in adults: a clinical practice guideline from the American College of Physicians. Hoge EA, Austin ED, Pollack MH (2007) Resilience: research evidence and conceptual considerations for posttraumatic stress disorder. service members returning from military deployments. McLay RN, Klam WP, Volkert SL (2010) Insomnia is the most commonly reported symptom and predicts other symptoms of post-traumatic stress disorder in U.S. Wright KM, Britt TW, Bliese PD, Adler AB, Picchioni D, Moore D (2011) Insomnia as predictor versus outcome of PTSD and depression among Iraq combat veterans. Īpplewhite L, Keller N, Borah A (2012) Mental health care use by soldiers conducting counterinsurgency operations. Hughes JM, Ulmer CS, Gierisch JM, Nicole Hastings S, Howard MO (2018) Insomnia in United States military veterans: an integrated theoretical model. Seelig AD, Jacobson IG, Smith B, Hooper TI, Boyko EJ, Gackstetter GD, Gehrman P, Macera CA, Smith TC, Millennium Cohort Study T (2010) Sleep patterns before, during, and after deployment to Iraq and Afghanistan. Īmin MM, Parisi JA, Gold MS, Gold AR (2010) War-related illness symptoms among operation Iraqi freedom/operation enduring freedom returnees. Maher MJ, Rego SA, Asnis GM (2006) Sleep disturbances in patients with post-traumatic stress disorder: epidemiology, impact and approaches to management. Future studies should examine whether racial and cultural influences on the generation of insomnia in veterans with PTSD affects the response to CBT-I.īaird T, McLeay S, Harvey W, Theal R, Law D, O'Sullivan R, Initiative P (2018) Sleep disturbances in Australian Vietnam veterans with and without posttraumatic stress disorder.  
While CBT-I ameliorates insomnia in veterans with PTSD, the use of hypnotics prior to instituting behavioral therapy may negatively affect the response rate to CBT-I. Younger age, non-white race, and use of hypnotics prior to behavioral therapy were independently associated with lack of response to CBT-I. In contrast to hypnotics, antidepressants usage decreased in those who had experienced benefit from CBT-I ( p = 0.001). Lack of perceived benefit was the most given reason for failure to return for follow-up. Seventy-seven percent completed treatment. ResultsĬBT-I responsiveness was observed in 47% of veterans with PTSD. A 6-point reduction or greater in ISI scores at 6-month follow-up visit was defined as CBT-I responsiveness. We converted prescribed antidepressant and hypnotic dosages before and after CBT-I to dose equivalent of fluoxetine diazepam, respectively. Epworth Sleepiness Score (ESS), PTSD Checklist (PCL), and Insomnia Severity Index (ISI) were assessed at baseline. MethodsĪ retrospective chart review of 136 veterans with PTSD-related insomnia was conducted. 
The aim of this study was to identify factors that may predict clinical response to CBT for insomnia (CBT-I) in veterans with PTSD.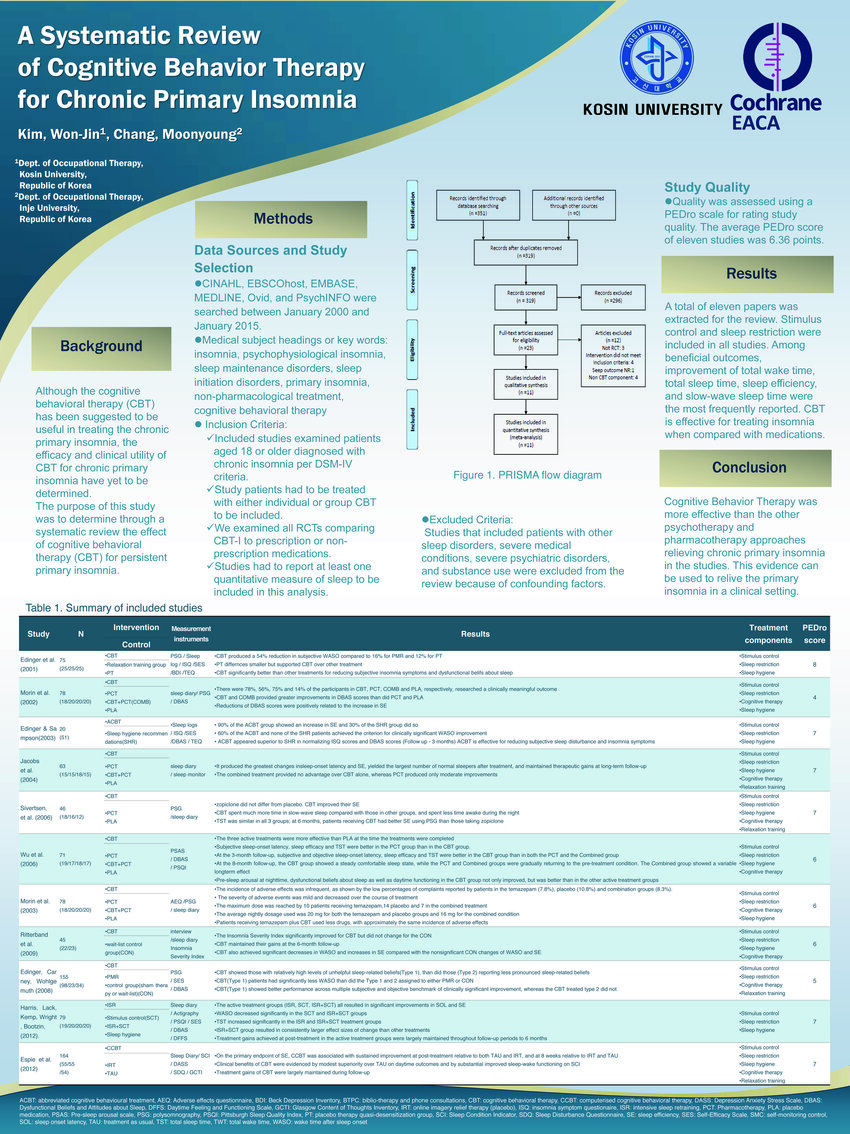 
Cognitive behavioral therapy (CBT) is considered an efficacious treatment, yet little attention has been devoted to treatment response in this population. Insomnia is a well-recognized co-morbid condition in veterans with post-traumatic stress disorder (PTSD) with negative personal and social consequences. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
